What is Gastro intestinal Surgery?
Gastrointestinal surgery, also known as GI surgery or gastrointestinal surgery, refers to surgical procedures that involve the organs of the gastrointestinal (GI) tract. The GI tract is a system of organs responsible for the digestion and absorption of food, as well as the elimination of waste. It includes various organs, such as the esophagus, stomach, small intestine, large intestine (colon), rectum, liver, gallbladder, and pancreas.
Types of minimally gastro intestinal surgery
Minimally invasive gastrointestinal surgery involves using techniques that result in smaller incisions compared to traditional open surgery. This approach aims to reduce trauma to the body, speed up recovery, and minimize scarring. Some common types of minimally invasive gastrointestinal surgeries include:
Laparoscopic Surgery:
- Laparoscopic surgery involves making several small incisions in the abdominal wall.
- A laparoscope (a thin, flexible tube with a camera) and specialized instruments are inserted through these incisions.
- The surgeon performs the procedure while viewing the internal structures on a monitor.
Robotic-Assisted Surgery:
- Robotic surgery combines advanced technology with a minimally invasive approach.
- The surgeon controls a robotic system that uses robotic arms to manipulate instruments with precision.
- Robotic-assisted surgery can be used for various gastrointestinal procedures, including colorectal surgery and pancreatic surgery.
Single-Incision Laparoscopic Surgery (SILS):
- SILS, also known as single-port laparoscopy, involves making just one small incision, typically in the navel.
- All instruments and the laparoscope are inserted through this single incision.
- SILS aims to further reduce the number of visible scars.
Natural Orifice Transluminal Endoscopic Surgery (NOTES):
- NOTES is an emerging technique that involves accessing the abdominal cavity through natural body openings, such as the mouth, anus, or vagina.
- Instruments are introduced through these natural orifices to perform surgery internally, avoiding external incisions.
- NOTES is still in the early stages of development and is not yet widely adopted.
Endoscopic Surgery:
- Endoscopic procedures use a flexible tube with a light and camera (endoscope) to visualize and treat conditions within the gastrointestinal tract.
- Endoscopic surgery is often used for conditions such as polyp removal, tumor biopsy, and treatment of gastrointestinal bleeding.
Transanal Minimally Invasive Surgery (TAMIS):
- TAMIS is a technique used for rectal surgery, specifically for removing polyps or early-stage rectal tumors.
- It involves accessing the rectum through the anus using specialized instruments.
The choice of the specific minimally invasive technique depends on various factors, including the nature of the gastrointestinal condition, the patient’s overall health, and the surgeon’s expertise. While these approaches offer benefits such as reduced pain, quicker recovery, and smaller scars, not all gastrointestinal surgeries are suitable for minimally invasive techniques, and the decision is made based on individual patient considerations.
What Are the Benefits of Minimally gastro intestinal surgery?
Smaller Incisions:
- Smaller incisions lead to less tissue trauma, reduced scarring, and a more aesthetically pleasing result.
Reduced Postoperative Pain:
- Patients undergoing minimally invasive surgery often experience less postoperative pain compared to those undergoing open surgery.
- Smaller incisions and decreased tissue manipulation contribute to reduced discomfort.
Quicker Recovery Time:
- Minimally invasive procedures generally result in a faster recovery and shorter hospital stays.
- Patients may return to normal activities sooner than those who undergo traditional open surgery.
Shorter Hospital Stay:
- Minimally invasive surgeries often allow for a shorter hospitalization, sometimes even allowing patients to go home on the same day or within a short period.
Lower Risk of Infections:
- Smaller incisions reduce the risk of postoperative infections and complications.
- Patients may experience a quicker return to normal immune function.
Improved Cosmetic Outcome:
- Reduced scarring and smaller incisions contribute to a more favorable cosmetic outcome.
- The cosmetic benefits are particularly relevant for procedures like single-incision laparoscopic surgery (SILS) and robotic-assisted surgery.
Less Blood Loss:
- Minimally invasive techniques often result in less blood loss during surgery.
- This can be particularly important for patients who may be at higher risk of complications related to blood loss.
Decreased Need for Pain Medications:
- Because patients often experience less pain after minimally invasive surgery, there may be a reduced need for postoperative pain medications.
Quicker Return to Normal Diet:
- Patients undergoing minimally invasive gastrointestinal surgery may resume a normal diet sooner compared to those who undergo open surgery.
It’s important to note that the suitability of minimally invasive surgery depends on various factors, including the specific gastrointestinal condition, the patient’s overall health, and the surgeon’s expertise. While minimally invasive approaches offer numerous benefits, not all gastrointestinal surgeries can be performed using these techniques, and the choice of the surgical approach is made based on individual patient considerations.
What Happens During Minimally gastro intestinal surgery?
The specific details of minimally invasive gastrointestinal surgery can vary depending on the type of procedure and the patient’s condition. However, here is a general overview of what typically happens during minimally invasive gastrointestinal surgery:
Preoperative Preparation:
- Before surgery, the patient undergoes a thorough preoperative assessment, which may include blood tests, imaging studies, and other diagnostic evaluations.
- Patients are often instructed to refrain from eating or drinking for a specified period before the surgery.
Anesthesia:
- The patient is given anesthesia to induce unconsciousness and ensure they do not feel pain during the surgery.
Incisions:
- Minimally invasive surgery involves making small incisions, often less than an inch in length.
- The number and location of the incisions depend on the specific procedure and the approach chosen (laparoscopic, robotic-assisted, single-incision, etc.).
Insertion of Instruments:
- Specialized instruments, including a laparoscope (a thin tube with a camera), are inserted through the small incisions.
- The laparoscope provides a video feed of the internal structures, allowing the surgeon to visualize the area being operated on.
Surgical Procedure:
- The surgeon performs the necessary steps of the procedure using the instruments inserted through the small incisions.
- Tissue manipulation, cutting, suturing, and other surgical tasks are carried out under the guidance of the laparoscope.
Closure of Incisions:
- Once the procedure is completed, the instruments are removed, and the small incisions are closed.
- Closure may involve sutures, staples, or adhesive strips.
Recovery and Observation:
- The patient is taken to the recovery room, where they are closely monitored as they wake up from anesthesia.
- Vital signs such as heart rate, blood pressure, and oxygen saturation are monitored.
- Pain management and other postoperative care measures are initiated.
Hospital Stay and Follow-up:
- Depending on the type of surgery and the patient’s condition, a hospital stay may be necessary for observation and recovery.
- Follow-up appointments are scheduled to monitor the patient’s progress and address any concerns.
Minimally invasive gastrointestinal surgery aims to minimize trauma to the body, reduce postoperative pain, and speed up recovery compared to traditional open surgery. The specific steps and techniques used will depend on the nature of the gastrointestinal condition being treated and the chosen approach (laparoscopic, robotic-assisted, etc.). It’s important for patients to follow preoperative and postoperative instructions provided by their healthcare team to optimize the surgical outcome.
What Are the Types of Minimally gastro intestinal surgery?
Laparoscopic Appendectomy:
- This procedure involves the removal of the appendix using small incisions and a laparoscope. It is commonly performed to treat appendicitis.
Laparoscopic Cholecystectomy:
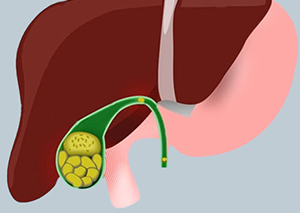
- This surgery is performed to remove the gallbladder, often due to gallstones or gallbladder inflammation.
Laparoscopic Colectomy:
- Colectomy is the removal of part or all of the colon. Laparoscopic colectomy is used for conditions such as colon cancer, diverticulitis, or inflammatory bowel disease.
Laparoscopic Nissen Fundoplication:
- This surgery is performed to treat severe gastroesophageal reflux disease (GERD). It involves wrapping the top of the stomach around the lower esophagus to prevent acid reflux.
Laparoscopic Hernia Repair:
- Hernias in the abdominal wall, such as inguinal or ventral hernias, can be repaired using laparoscopic techniques.
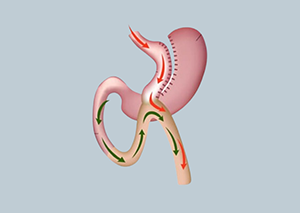
Laparoscopic Sleeve Gastrectomy:
- This is a type of weight loss surgery that involves removing a portion of the stomach to reduce its size and limit food intake.
Robotic-Assisted Colorectal Surgery:
- Robotic systems are sometimes used to assist in colorectal procedures, including colectomy and rectal surgery. The surgeon controls a robotic system to perform precise movements.
Single-Incision Laparoscopic Surgery (SILS):
- SILS involves performing various gastrointestinal procedures through a single incision, usually in the navel. It aims to reduce visible scarring.
Transanal Minimally Invasive Surgery (TAMIS):
- TAMIS is used for rectal surgery, particularly for the removal of polyps or early-stage rectal tumors. It involves accessing the rectum through the anus.
Endoscopic Surgery:
- Various endoscopic procedures are used for diagnostic and therapeutic purposes. Examples include endoscopic removal of polyps, endoscopic mucosal resection (EMR), and endoscopic submucosal dissection (ESD).
It’s important to note that the choice of minimally invasive technique depends on factors such as the specific gastrointestinal condition, the location of the problem, the patient’s overall health, and the surgeon’s expertise. While these procedures offer benefits such as smaller incisions, reduced pain, and quicker recovery, not all gastrointestinal surgeries are suitable for minimally invasive approaches, and the decision is made on a case-by-case basis.